Syncope toolkit
Syncope is very common and will affect 42% of people during their lifetime
Investigations
In this section:
- Electrocardiogram (ECG)
- Blood tests
- Active stand test
- 24-hour ambulatory and home blood pressure monitoring (ABPM, HBPM)
- Holter monitor
- Implantable cardiac monitor (ICM) previously known as insertable loop recorder (ILR)
- Tilt table test
- Autonomic tests
- Exercise testing
- Tests of low clinical value
- Syncope of unknown origin case history.
Electrocardiogram (ECG)
All patients with an unexplained blackout should have a 12 lead ECG with automated interpretation. If this is unavailable, a manual ECG should be recorded and analysed by a healthcare professional who is trained and competent at reading ECGs.
ECGs patterns in children and adolescents can vary with age and are different from those of adults.
Reasons to use ECGs:
- European Society of Cardiology guidelines for the diagnosis and management of syncope recommend ECG as the first investigation for syncope
- A comprehensive history, examination (including postural blood pressure measurements) and ECG can diagnose a cause of syncope in 23-50% of patients
- ECGs are a non-invasive, inexpensive tool for identifying a cause and helping guide prognosis and risk stratification.
What an ECG can tell you in syncope:
- ECGs are more likely to identify ischaemic, structural or conduction abnormalities than arrhythmias, many of which are paroxysmal
- Abnormal ECG findings occur in 90% of patients with cardiac-induced syncope but in only 6% of patients with vasovagal syncope
- A normal ECG makes it unlikely that an arrhythmia is the cause of syncope, and these persons are at low risk of sudden death
- A normal ECG can be helpful in reducing the need for further investigations including echocardiography.
ECG red flags in syncope
The following are examples of ECGs that are red flags in syncope and should prompt consideration of urgent assessment of the patient presenting with syncope.
- Sinus bradycardia
- Sinus pauses/prolonged asystole
- AV block – 2nd degree (types 1, 2) and complete heart block
- Bundle branch blocks - right and left bundle branch block and 'trifasicular' block
- Atrial fibrillation and atrial flutter
- Wolf-Parkinson-White syndrome
- SVT
- Ventricular tachycardia, Torsades de Pointes and ventricular fibrillation
- Long QT
- Short QT
- Brugada syndrome
- ARVC
- Ischaemic heart disease ef anterior myocardial infarction, old inferior myocardial infarction
- ST-T wave changes
- Left ventricular hypertrophy (LVH) or right ventricular hypertrophy
- Pulmonary embolism
- Pacemaker malfunction.
We would like to thank Dr Dean Jenkins, Stephen Gerred and Prof Richard Sutton for providing these images. Further ECG images can be found on ECG Library.
Blood tests
Consider the following points about blood tests:
- Routine blood tests are rarely cost effective in adults with syncope unless guided by clues in the history suggesting an underlying diagnosis, for example diabetes or gastrointestinal (GI) blood loss
- It can be helpful to check for iron deficiency in children
- May be helpful in detecting metabolic abnormalities such as electrolyte abnormalities to explain loss of consciousness if witness account not available
- Some studies have proposed a role for using B-type natriuretic peptide (BNP) or high sensitivity Troponin I, which add evidence of the existence of structural heart disease for predicting adverse outcomes in syncope, but it is too early to recommend for routine clinical practice.
Active stand test
The active stand test is sometimes called ‘the poor man’s tilt table test’ by patients. It is useful in identification of orthostatic hypotension (classic and immediate types), and PoTS (when it may also be called 'the 10 minute NASA learn test').
How the active stand test works:
- The patient is rested supine, then asked to stand up (ideally against a wall or in front of a chair to minimise injury if the patient starts to feel faint)
- A manual or battery-operated sphygmomanometer can be used to repeatedly record heart rate and blood pressure whilst supine then for a minimum of 3 and up to 10 minutes while standing.
Continuous beat-to-beat non-invasive blood pressure and heart rate monitoring in a laboratory in secondary care will yield more detailed information than a manual blood pressure monitor and may be performed in conjunction with a tilt test. Active stand employs the leg muscle pumps while tilt testing does not and therefore they reveal different haemodynamic effects.
24-hour ambulatory and home blood pressure monitoring (ABPM, HBPM)
Points to consider with ABPM and HBPM:
- May be useful to investigate unexplained syncope especially in older patients with one study showing 25% of elderly patients admitted with falls or syncope had post-prandial hypotension especially after breakfast.
- ABPM is recommended to detect a degree of orthostatic hypotension, supine hypertension and nocturnal hypertension in patients with autonomic failure.
- ABPM and HBPM may be considered to detect whether blood pressure is abnormally low during episodes suggestive of orthostatic intolerance. A symptom diary during monitoring can be helpful.
- ABPM may be more useful than tilt table testing to evaluate orthostatic hypotension.
- ABPM can evaluate BP over a longer time period than tilt table testing, counteract the effect of white coat hypertension and provide insight into blood pressure variations during the day which may be influenced by food, posture and medication. ABPM can also be useful to detect overtreatment of hypertension which can result in syncope, but its limitation is the relative infrequency of BP measurements.
Holter monitor
Holter monitors are of limited value and only useful if syncope or presyncope symptoms are very frequent, for example daily. Other points to note:
- Holter monitors allow continuous ECG monitoring from 24-48 hours to 1-2 weeks.
- 24-hour Holter monitoring is of limited benefit due to the short duration of monitoring and ECG rhythm and symptom correlation is rarely achieved. 24-hour Holter monitoring should be considered in patients who have frequent (ideally daily) episodes.
- Diagnostic yield is reported to be as low as 1-2% in unselected patients.
- They have a greater sensitivity in achieving diagnosis in those with cardiac syncope but the frequency of events must be high and this suggests a need for in-hospital monitoring.
- Normal Holter monitoring does not exclude arrhythmia as a cause of syncope if no event occurs.
- Holter monitoring may show evidence of arrhythmias in normal, asymptomatic individuals.
- Extending monitoring to 72 hours increases the number of asymptomatic arrhythmias detected but not overall diagnostic yield.
- Prolonged external loop recording, for example 14 days, has a higher diagnostic yield than conventional Holter monitoring, forming an interim strategy between Holter and implantable cardiac monitor.
Implantable cardiac monitor (ICM) previously known as insertable loop recorder (ILR)
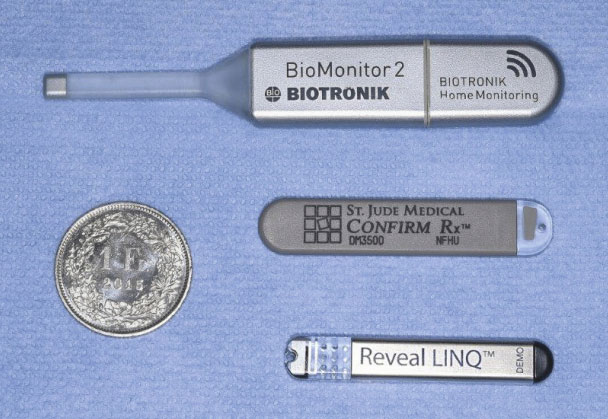
Image courtesy of Dr Alexander Breitenstein, Journal of Cardiovascular Medicine.
The ICM is a small device which is implanted subcutaneously within the chest wall and monitors heart rate continuously. They are designed to record abnormal heart rhythms and can remain under the skin for up to four years.
Indications
- In suspected reflex syncope, where the diagnosis is not clear after initial evaluation
- In patients with suspected cardiac cause of syncope, consider if syncope is less frequent than every 1-2 weeks
- Suspected epilepsy where arrythmia should be excluded
- Unexplained falls
- Inherited arrhythmia disorders or primary cardiomyopathy where there is low risk of cardiac death (alternative to ICD)
- ICMs are valuable in detecting infrequent arrhythmias and can be programmed for automatic and patient activated detection.
Insertion
ICMs can be inserted just underneath the skin over the chest wall, usually close to the left sternal edge, via a minimally invasive procedure. They have no external parts and can transmit data to a diagnostic station via automatic or simple patient demand. Implantation is associated with a low rate of infection (1-4%). Although currently they are mostly inserted in a hospital setting, they have occasionally been implanted by GPs in their surgery.
Advantages of ICM
The advantages of ICM include:
- Long term ECG monitoring with an ICM extends the monitoring period up to four years compared with the very short period of Holter monitoring, reduces patient non-compliance and does not prohibit physical activity
- Early use of ICM enables treatment, including pacing, to be delivered more safely, specifically and effectively
- Use of ICMs reduces the number of A&E attendance in patients with recurrent syncope.
Diagnostic yield
ICMs have been found to be more cost effective than conventional strategies and are more likely to provide a diagnosis in patients with recurrent unexplained syncope.
The estimated diagnostic yield of the following investigations used in syncope is:
- 1–5% for a 24–48 hour standard Holter monitor
- 5–10% for a 3–7 day external ECG or event recorder
- 15–25% for a 1–4 week external ECG or event recorder
- 30–50% for a ≤ 36 month ICM
- 80% for 48 months.
ICMs have higher diagnostic rates in older patients and can provide a diagnosis in 20% of patients aged over 50 with unexplained recurrent falls and normal initial cardiac evaluation.
Tilt table test
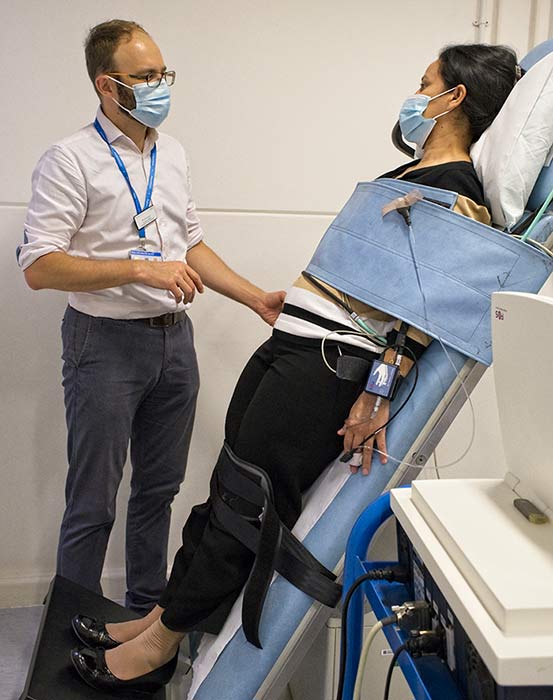
Image courtesy of Syncope Unit at Hammersmith Hospital, Imperial College Healthcare NHS Trust.
Procedure
The tilt table test is performed in a room where resuscitation equipment is rapidly available. The patient lies supine on a tilting bed with a footplate and straps. The test starts with the patient resting still in a supine position for between five and over 20 minutes, and then is tilted head up to 60-70 degrees for approximately 20-45 minutes.
If there is no response, sublingual GTN spray or an isoproterenol infusion may be administered. Carotid sinus massage may be performed in patients over 40 years of age. The patient is monitored throughout and either syncope is induced, or the test protocol is completed.
Points to consider with the tilt table test:
- Tilt table testing is a more useful investigation than Holter monitoring in diagnosing suspected vasovagal syncope
- The test is time consuming and requires experienced staff and technical equipment, varies in its reproducibility and does not reproduce completely a spontaneous syncope
- Head-up tilt table testing is safe with very few reported adverse events.
The tilt table test helps to diagnose or differentiate between the following conditions:
- Atypical reflex syncope
- Orthostatic hypotension
- Postural tachycardia syndrome
- differentiating syncope with jerking movements and epilepsy especially when combined with video-EEG
- Frequent TLoC where psychogenic pseudosyncope is suspected
- Single syncopal episode in high-risk settings or in people who have recurrent syncopal episodes in the absence of heart disease
- Distinguishing syncope from recurrent falls
- Confirming vasovagal syncope, which gives improved patient confidence in the diagnosis and educates the patient in prodromal symptoms. It also provides an occasion to teach the patient physical countermeasures where their efficacy can be demonstrated.
Autonomic tests
Laboratory testing of the autonomic nervous system can help when autonomic dysfunction is the possible cause of syncope.
- The most widely used test of cardiac parasympathetic function is heart rate variability
- Heart rate responses to a Valsalva manoeuvre examine sympathetic function
- Common tests of sympathetic adrenergic function include the blood pressure response to postural change with tilt table testing and active standing
- Autonomic function testing provides a safe, effective way to further evaluate patients presenting with syncope and can be diagnostic for autonomic failure (for example pure autonomic failure, multisystem atrophy, Parkinson’s disease), classical and delayed orthostatic hypotension, vasovagal syncope, and PoTS.
Exercise testing
Exercise stress testing is indicated in patients whose syncope is related to exercise. The test involves the patient undertaking exercise (usually on a treadmill) whilst attached to an ECG monitor.
When syncope occurs during exercise, urgent exercise testing should be considered. Advise the patient to avoid exercise until seen by their secondary care specialist. Exercise testing is usually contraindicated in aortic stenosis and hypertrophic cardiomyopathy (these conditions can cause syncope on exercise).
- Unselective exercise testing delivers a poor diagnostic yield in the investigation of syncope
- Investigation with exercise stress testing can lead to the diagnosis of ischaemia or arrhythmias precipitated by exercise, in contrast to post-exertional vasovagal syncope that may be associated with autonomic dysfunction.
Tests of low clinical value
The following tests are of low diagnostic yield in syncope and should not routinely be offered unless specifically indicated:
- Brain imaging
- Carotid artery doppler
- Electroencephalogram (EEG)
- Chest x-ray
- Routine blood tests
- D Dimer
- Cardiac markers.
Tilt test – should not be offered to the patient with clear history of vasovagal syncope unless there is a strong need for confirming the diagnosis or for further patient education (see above).