_ RCGP Learning
Blog entry by _ RCGP Learning
Written by Dr Dirk Pilat
The NHS Bowel Cancer screening programme was first rolled out across the United Kingdom in 2006, using the guaiac faecal occult bood test (gFOBT). It was initially only offered to people between 60 and 70, but subsequently extended to 74 (patients over 75 can request tests if they would like to continue testing1). gFOBT was replaced from 2017 to 2021 across the NHS with the faecal immunochemical test (FIT) and extended to younger people2. The stool guaiac test had various issues: a long list of medications could potentially cause false positives, as could certain foods3. It was also trickier to use, as patients had to apply six dollops of faeces from three different bowel motions to a little paper envelope, reducing the acceptability of the test4. The FIT testing kit reduced this complexity and added improved acceptability to just a simple scrape of a testing stick across one faecal sample before adding it to a sample bottle5. As FIT uses antibodies to detect the presence of human blood, it is both more sensitive and specific than gFOBT6.
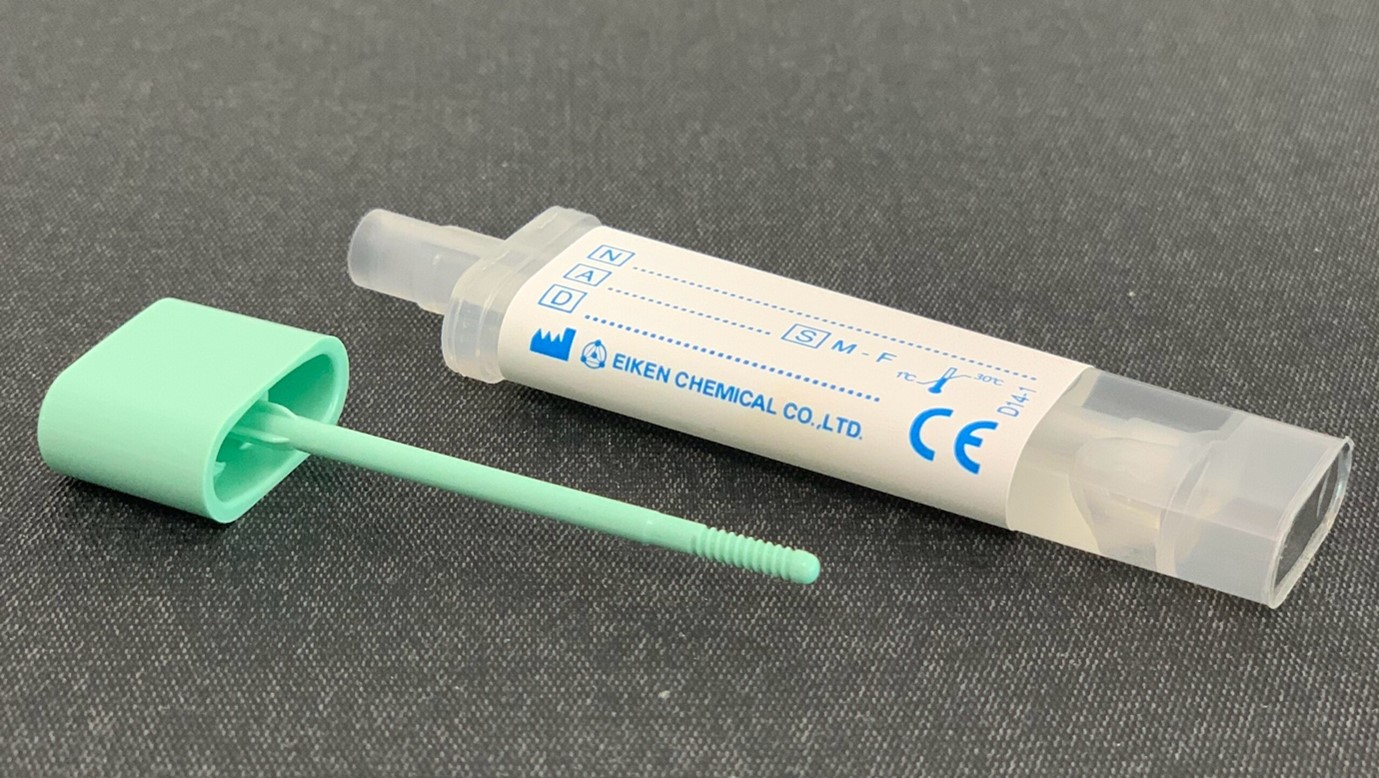
Figure 1 FIT sample container. By Whispyhistory - Own work, CC BY-SA 4.0,
The move to FIT caused an increase of screening uptake from under 60% to nearly 70%. Since the introduction of bowel cancer screening in England, the incidence of colorectal cancer in adults fell by 7%. For 2023 to 2024, NHS England:
- Invited 6,969,227 people to take part in screening
- 4,710,330 of them took up the offer of screening, an overall uptake of 67.6%
- 83,112 (1.76%) of the people screened were invited back for further tests
- screening led to 35,039 colonoscopies where at least one high risk polyp was detected
- 5,320 bowel cancers were found – a detection rate of 0.11%7.
Across England, Scotland and Wales, eligibility for bowel cancer screening starts at 50 and ends at 74, with biannual invitations. In Northern Ireland eligibility is from 60 to 748.
While the current FIT threshold for referral in England and Northern Ireland is 120 μg Hb/g, Wales has already lowered its threshold for referral to 80μg Hb/g and Scotland has always set its FIT threshold at 80μg Hb/g. In symptomatic patients who had their FIT arranged in primary care, NICE suggests to refer using a suspected cancer pathway referral for colorectal cancer if they have a FIT result of at least 10 micrograms of haemoglobin per gram of faeces9.

Figure 2 FIT instructions by Cancer Research UK
In 2026 the threshold in England is being lowered to 80μg Hb/g in a phased rollout that should be completed by March 2028. This will likely increase the amount of positive screening results by 36%, resulting in the detection of an extra 2017 high risk polyps and 663 more bowel cancers.
While bowel screening is not part of day to day general practice, we still have an important role to play: encouraging to take part in the screening activity by their general practitioner results in a significant increase in uptake10 and the use of our computerised patient management systems can help here, as we are being notified if patients are not participating.
We know that more than half of patients having to undergo a colonoscopy experience anxiety around the procedure. This is due to worries about bowel preparation, difficulties with the procedure (embarrassment, pain, possible complications, and sedation), and concerns about the diagnosis - including fear of being diagnosed with cancer11. With the increase in recalls, our patients’ concerns are likely going to lead to an increased amount of people contacting their primary care teams, fearful of going ahead with the examination. We can signpost our patients to a detailed (and reassuring) explanation of what happens on the day of their colonoscopy provided by the NHS here.
Reassurance from their primary care team can go a long way to allay a patient’s concerns and support them in partaking in this important screening programme.
References
- NHS. Bowel Cancer Screening. 2024.
- Whyte S, Sun Y. T. ModelHealth and Resource Consequences of Reducing the Faecal Immunochemical Test(FIT) Screening Threshold for Colonoscopy in the NHS Bowel Cancer Screening Programme (BCSP) [accessed February 2026].
- Kaur K, Zubair M, Adamski JJ. Fecal Occult Blood Test. December 2025 [accessed February 2026].
- Strachan H. Wealth of evidence highlights the benefits of bowel cancer screening UK National Screening Committee 2025. [accessed February 2026].
- Cancer research UK. Together we will beat cancer Tips for collecting your poo. [accessed February 2026].
- Alpha Laboratories. About Faecal Immunochemical Testing - What is a FIT?[accessed February 2026].
- Strachan H. Wealth of evidence highlights the benefits of bowel cancer screening UK National Screening Committee 2025. [accessed February 2026].
- Bowel Cancer UK. Bowel cancer screening | About bowel cancer. 2019. [accessed February 2026].
- NICE. Suspected cancer: recognition and referral. 2026. [accessed February 2026].
- Triantafillidis JK, Vagianos C, Gikas A, et al. Screening for colorectal cancer:the role of the primary care physician. European Journal of Gastroenterology & Hepatology. 2017 Jan 1; 29(1): e1–7. [accessed February 2026].
-
Yang C, Sriranjan V, Abou-Setta AM, et al. Anxiety Associated with Colonoscopy and Flexible Sigmoidoscopy: A Systematic Review. American Journal of Gastroenterology. 2018 Dec; 113 (12): 1810–8.